Anesthesia Subspecialties
The Anesthesiology specialties listed below are areas where our department has significant focus and involvement. There are additional areas of Anesthesiology specialization including transplant, chronic pain management, geriatrics, bariatrics, etc. for which we also provide care. For just about any area of surgical or procedural specialization there is an associated area of specialization in Anesthesiology primarily because each different type of surgery may involve a different subset of patients and different set of preoperative concerns, intra-operative requirements and clinical consequences. Long Island Anesthesiologists engages in ongoing efforts to build and maintain expertise in all areas of specialization where our services are requested. And individually, our physicians are committed to providing the highest standard of care in all our clinical settings. Please refer to our “Annual Clinical Initiatives” for more information about our ongoing quality improvement and academic endeavors.
Regional Anesthesia/Orthopedics
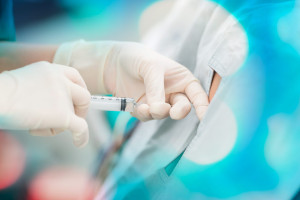 This area of specialization involves the use of extremity and spinal nerve blocks to eliminate sensation and movement from select “regions” of the body for the purposes of surgery, or to anesthetize partially a region of the body for the purpose of post-operative pain relief. Regional Anesthesia and nerve blocks are used for many types of surgery and may be combined with sedation, neuraxial or general anesthesia. Their use is especially common in the setting of orthopedic surgery. All of our anesthesiologists are skilled in routine regional anesthetic techniques and several of our physicians have advanced training in traditional and ultrasound guided regional anesthesia for surgery, perioperative pain relief and acute pain management.
This area of specialization involves the use of extremity and spinal nerve blocks to eliminate sensation and movement from select “regions” of the body for the purposes of surgery, or to anesthetize partially a region of the body for the purpose of post-operative pain relief. Regional Anesthesia and nerve blocks are used for many types of surgery and may be combined with sedation, neuraxial or general anesthesia. Their use is especially common in the setting of orthopedic surgery. All of our anesthesiologists are skilled in routine regional anesthetic techniques and several of our physicians have advanced training in traditional and ultrasound guided regional anesthesia for surgery, perioperative pain relief and acute pain management.
Pediatric Anesthesiology
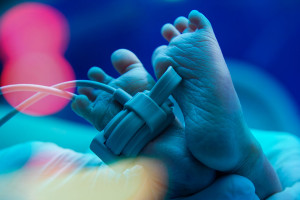 Pediatric Anesthesiology, like the field of Pediatrics, involves the care of young people from birth to age 21, and especially the care of babies, both in the setting of health and illness. Young people at each developmental stage have a unique set of pathologic, physiologic, emotional and behavioral factors affecting their health and responses to illness, surgery and anesthetics. While all Anesthesiologists provide routine and emergency care for children of many ages, Pediatric Anesthesiologists obtain advanced or fellowship training that prepares them to care for our youngest patients, from prematurity on, for both routine surgical problems and critical illness. Pediatric Anesthesiologists specialize in providing age appropriate patient interactions and anesthetics. In relation to age appropriate care, all anesthetic techniques available to adults may be used in the pediatric setting, and all of our Anesthesiologists are experienced in providing care to pediatric patients. Leading these efforts are seven full time Pediatric Anesthesiologists. These dedicated professionals set the standard for pediatric care in our department, provide the bulk of our pediatric anesthetics, offer assistance and consultation as needed with all our pediatric patients, and specifically deliver the care for our very youngest patients. Please see “What to expect for the Pediatric patient.” for more information.
Pediatric Anesthesiology, like the field of Pediatrics, involves the care of young people from birth to age 21, and especially the care of babies, both in the setting of health and illness. Young people at each developmental stage have a unique set of pathologic, physiologic, emotional and behavioral factors affecting their health and responses to illness, surgery and anesthetics. While all Anesthesiologists provide routine and emergency care for children of many ages, Pediatric Anesthesiologists obtain advanced or fellowship training that prepares them to care for our youngest patients, from prematurity on, for both routine surgical problems and critical illness. Pediatric Anesthesiologists specialize in providing age appropriate patient interactions and anesthetics. In relation to age appropriate care, all anesthetic techniques available to adults may be used in the pediatric setting, and all of our Anesthesiologists are experienced in providing care to pediatric patients. Leading these efforts are seven full time Pediatric Anesthesiologists. These dedicated professionals set the standard for pediatric care in our department, provide the bulk of our pediatric anesthetics, offer assistance and consultation as needed with all our pediatric patients, and specifically deliver the care for our very youngest patients. Please see “What to expect for the Pediatric patient.” for more information. Obstetric Anesthesiology
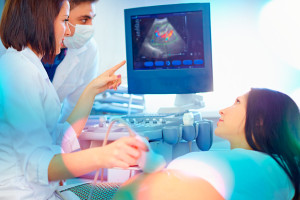 Obstetric Anesthesia involves the care of pregnant women and secondarily their developing children. Pregnant woman may face the need for surgery or anesthesia in relation to the pregnancy itself, or for issues unrelated to the pregnancy such as appendicitis, cholecystitis or trauma at any time during a typical nine month gestation. Additionally, many woman either choose or require anesthetics for labor and delivery. It is fair to say that the period around delivery is the main focus of the Obstetric Anesthesiologist and you can feel confident that our entire department is skilled in this area of practice and regularly involved in the care of pregnant woman. At our central practice location, Good Samaritan Hospital, we offer 24/7 in-house Obstetric Anesthesia coverage for thousands of deliveries each year, both routine and high risk. Please see “What to expect for the Obstetric patient.” for further information.
Obstetric Anesthesia involves the care of pregnant women and secondarily their developing children. Pregnant woman may face the need for surgery or anesthesia in relation to the pregnancy itself, or for issues unrelated to the pregnancy such as appendicitis, cholecystitis or trauma at any time during a typical nine month gestation. Additionally, many woman either choose or require anesthetics for labor and delivery. It is fair to say that the period around delivery is the main focus of the Obstetric Anesthesiologist and you can feel confident that our entire department is skilled in this area of practice and regularly involved in the care of pregnant woman. At our central practice location, Good Samaritan Hospital, we offer 24/7 in-house Obstetric Anesthesia coverage for thousands of deliveries each year, both routine and high risk. Please see “What to expect for the Obstetric patient.” for further information. Neuroanesthesiology
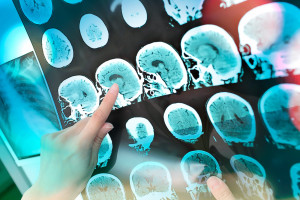 Specialized anesthesia for neurosurgery relates primarily to surgeries or procedures around the brain and spinal cord. In our department, these surgeries include major and minor spine surgery, pediatric scoliosis repair, cranial surgeries possibly related to hemorrhage, trauma or tumors, and procedures for the treatment of chronic pain. Specialized monitoring and anesthetic techniques are used in these cases for neuroprotection and to help patients achieve the best outcomes possible. Our department includes members who have trained and worked as Neuroanesthesiologists at some of the busiest neurosurgical centers in the area, and all of our Anesthesiologists regularly care for neurosurgical patients.
Specialized anesthesia for neurosurgery relates primarily to surgeries or procedures around the brain and spinal cord. In our department, these surgeries include major and minor spine surgery, pediatric scoliosis repair, cranial surgeries possibly related to hemorrhage, trauma or tumors, and procedures for the treatment of chronic pain. Specialized monitoring and anesthetic techniques are used in these cases for neuroprotection and to help patients achieve the best outcomes possible. Our department includes members who have trained and worked as Neuroanesthesiologists at some of the busiest neurosurgical centers in the area, and all of our Anesthesiologists regularly care for neurosurgical patients. Cardiothoracic and Vascular Anesthesia
 Cardiothoracic Anesthesia concerns surgery inside the chest cavity. These surgeries mainly involve the heart or lungs, but also at times the surrounding blood vessels, lymph nodes and chest wall. Anesthetic care for these patients includes the use of sedation, regional and general anesthetics as well as advanced techniques for vascular access, monitoring and pain management. It requires specialized understanding of related cardiopulmonary physiology and the effects and risks associated with intrathoracic or intracardiac procedures. Members of our department are experienced and trained in all major aspects of cardiothoracic surgery. Currently our practice involves us in the care of patients for surgeries of the lung, chest wall and mediastinum, and cardiac electrophysiologic procedures of both the left and right heart.
Cardiothoracic Anesthesia concerns surgery inside the chest cavity. These surgeries mainly involve the heart or lungs, but also at times the surrounding blood vessels, lymph nodes and chest wall. Anesthetic care for these patients includes the use of sedation, regional and general anesthetics as well as advanced techniques for vascular access, monitoring and pain management. It requires specialized understanding of related cardiopulmonary physiology and the effects and risks associated with intrathoracic or intracardiac procedures. Members of our department are experienced and trained in all major aspects of cardiothoracic surgery. Currently our practice involves us in the care of patients for surgeries of the lung, chest wall and mediastinum, and cardiac electrophysiologic procedures of both the left and right heart.
Our department is also routinely involved in the care of patients for major and minor vascular surgery. These procedures range from vein stripping to carotid endarterectomy to both open and endovascular repair of abdominal aortic aneurysms. In general, patients with systemic and peripheral vascular disease carry with them a cluster of medical issues requiring broad knowledge and skill from the anesthesiologists involved in their care. We are fortunate and privileged to work with an active vascular surgery service through which our department maintains a cutting edge ability to care for these patients, and a broad understanding of the perioperative issues that often accompany vascular surgery.
Critical Care Anesthesia
 Much of general Anesthesiology practice involves critical or intensive care. Life sustaining and life saving measures are regularly provided in the operating room. Also, the Post Anesthesia Care Unit (PACU) or recovery room is considered an intensive area and functions as an extension of the ICU. All anesthesiologists spend a considerable amount of their training taking care of patients in intensive care units. Additionally, our department has anesthesiologists who have obtained further training and board certification in Critical Care allowing them to provide care to patients beyond the PACU and through the duration of critical illness. These members of our physician team help to maintain and advance the practice of Critical Care Medicine throughout our practice both in and out of the hospital.
Much of general Anesthesiology practice involves critical or intensive care. Life sustaining and life saving measures are regularly provided in the operating room. Also, the Post Anesthesia Care Unit (PACU) or recovery room is considered an intensive area and functions as an extension of the ICU. All anesthesiologists spend a considerable amount of their training taking care of patients in intensive care units. Additionally, our department has anesthesiologists who have obtained further training and board certification in Critical Care allowing them to provide care to patients beyond the PACU and through the duration of critical illness. These members of our physician team help to maintain and advance the practice of Critical Care Medicine throughout our practice both in and out of the hospital.
Ambulatory Anesthesia / Day Surgery
 Many surgical procedures can now be done on an outpatient basis, allowing patients to return home on the day of surgery. The goal of sending patients home after surgery presents both benefits and limitations. All our Anesthesiologists are experienced with ambulatory surgical care and first evaluate patients medically for the appropriateness and safety of their return home on the day of surgery. In discussion and cooperation with the surgeon, they then craft and manage their anesthetics with the goals of rapid recovery, safety and optimal pain relief, limiting the need for post operative narcotics. These techniques may involve sedation, general and regional anesthesia, nerve blocks and the use of adjuvant analgesics. After the surgery or procedure is over, our Anesthesiologists reevaluate all patients prior to their discharge home. As a department we work in hospital ambulatory surgery units, free standing surgery centers and physicians’ offices. We are experienced in all these settings, with the issues facing ambulatory surgery patients, and also with the logistics and management of office set-ups and regulatory compliance.
Many surgical procedures can now be done on an outpatient basis, allowing patients to return home on the day of surgery. The goal of sending patients home after surgery presents both benefits and limitations. All our Anesthesiologists are experienced with ambulatory surgical care and first evaluate patients medically for the appropriateness and safety of their return home on the day of surgery. In discussion and cooperation with the surgeon, they then craft and manage their anesthetics with the goals of rapid recovery, safety and optimal pain relief, limiting the need for post operative narcotics. These techniques may involve sedation, general and regional anesthesia, nerve blocks and the use of adjuvant analgesics. After the surgery or procedure is over, our Anesthesiologists reevaluate all patients prior to their discharge home. As a department we work in hospital ambulatory surgery units, free standing surgery centers and physicians’ offices. We are experienced in all these settings, with the issues facing ambulatory surgery patients, and also with the logistics and management of office set-ups and regulatory compliance. Post-operative Pain Management / The Acute Pain Service
 Acute Pain Management is primarily concerned with providing optimal relief from pain in the immediate period and first few days after surgery. Our Anesthesiologists have the additional goal of facilitating full and rapid recovery from the surgery itself. Surgical recovery may require limiting the use of medications that limit movement or have systemic side effects such as sedation, decreased bowel motility or confusion. Our physicians and dedicated nurse practitioner on our Acute Pain Service work closely with surgeons and patients to strike the best possible balance between these sometimes competing needs. There are several modalities used to adapt our post operative pain management to your needs:
Acute Pain Management is primarily concerned with providing optimal relief from pain in the immediate period and first few days after surgery. Our Anesthesiologists have the additional goal of facilitating full and rapid recovery from the surgery itself. Surgical recovery may require limiting the use of medications that limit movement or have systemic side effects such as sedation, decreased bowel motility or confusion. Our physicians and dedicated nurse practitioner on our Acute Pain Service work closely with surgeons and patients to strike the best possible balance between these sometimes competing needs. There are several modalities used to adapt our post operative pain management to your needs:– Preoperative medication initiation
– Intra-operative preconditioning
– IV PCA
– Single Shot, Continuous or patient controlled Epidural Analgesia
– Single Shot or Continuous Peripheral Nerve Blocks
– Abdominal Wall Blocks
– optimized adjuvant analgesics
One or more of these methods may be used simultaneously. Patients are seen by the Acute Pain Management Service on the day of surgery and daily thereafter until their pain has diminished or becomes manageable by standard oral analgesic regimens.

